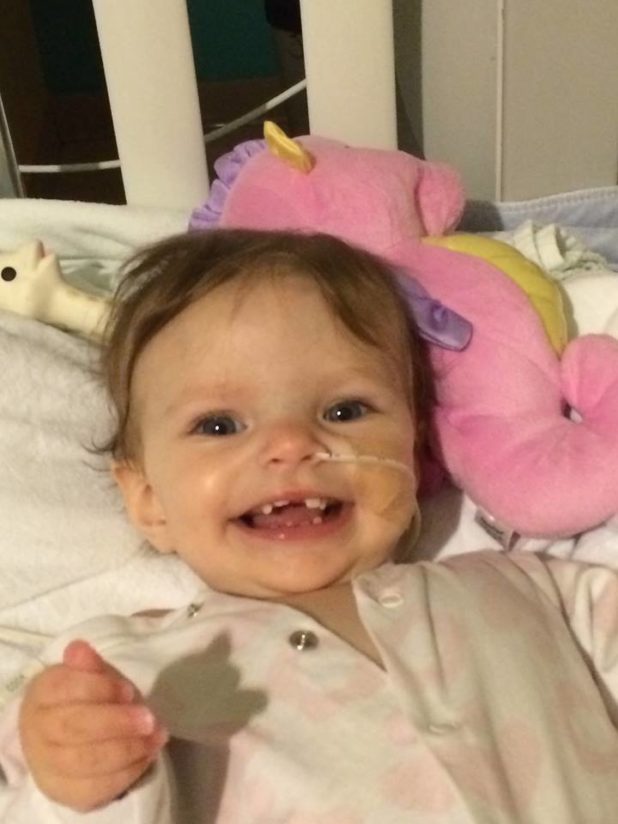
The following are words from Natasha’s mom, Vanessa. As she explains in an interview prior to her family’s participation in the 2017 Simon’s Cycles YANA Ride, “When you lose a child, the hardest thing is for them to be forgotten. You want their journey to matter.” Sharing Natasha’s story, donating her tricycle to another YANA child and taking part in the YANA Ride are contributing to this family’s healing.
Natasha Rose, was born a healthy baby, from an uncomplicated pregnancy. She was a normal length and the exact same weight at birth as her big brother at birth.
At just two-months-old, after her two-month check-up, she was referred to a pediatrician to rule out a suspected hip dysplasia. After careful examination, the doctor confirmed that her hips were normal and she was healthy, but he wanted to follow up in a month.
On the next visit, hip dysplasia was completely ruled out, but the doctor noticed that Natasha wasn’t gaining weight at a normal rate. She appeared to be fine otherwise, but he ordered some tests to rule out a few issues and we were to visit again in two weeks.
The tests came back fairly normal, but Natasha’s spleen and liver were enlarged and she still wasn’t growing at a sufficient rate and by now, she had been restless and sweaty at night. The doctor believed that she had something called Storage Disease, a genetic defect that prevents the body from properly breaking down and absorbing nutrients. He wanted more tests and time to look into the disease.
Now, four-months-old, Natasha seemed like a normal healthy and happy baby. We weren’t too concerned about her health. We thought her restless sleep was due to gas and with the help of probiotics, she began to feel and sleep better. We visited the doctor again, and this time, we felt confident that everything would be back to normal and we could get on with enjoying our happy little girl. He was pretty confident that it wasn’t Storage Disease by this point and he examined her thoroughly, though he was bothered still by her slow weight gain and growth and recorded it as failure to thrive, but why? Her liver and spleen were still slightly enlarged, but not as bad as before, but something just wasn’t right.
Then he heard it, he was so angry with himself, why hadn’t he noticed it before? Natasha had an irregular heart beat. It would come and go and almost always be normal but every once in a while he could hear the irregularity. He didn’t want to take any chances, he wanted us to go straight to Victoria General Hospital to have something called an Echocardiogram done by a pediatric cardiologist. These were all bizzare, unfamiliar terms to us, but we agreed that it was probably nothing, but better to rule everything out.
So we went to Victoria, feeling pretty confident that this test would come back normal and we could carry on worry free. We decided that our overnight trip to Victoria could be fun, after the little test, maybe we’d look around a bit before driving home. Our neighbour, who was a regular volunteer with YANA suggested that we contact them for support, and travel assistance. We did, though we felt kind of guilty since Natasha wasn’t really sick, it was just a simple test and we’d be back home the next day. That’s when Natasha’s whole life was turned upside down and things were forever changed.
We met with the cardiologist in the morning and he and his colleague conducted the echo test, which is basically an ultrasound of the heart. It can examine the structure, strength and efficiency of the heart and give a detailed view of any issues. The test was pretty quick and easy and we were asked to wait until the cardiologist could come back to chat with us. After a ten-minute wait, he invited us into his office and said: “We need to talk.”
I remember sitting in that waiting room seeing all of the sick kids and their worried families, thinking: “It must be so hard to have a child who is sick having to go through terrible procedures. Thank goodness there are so many organizations to help them through it.” I remember thinking how awful it must be to have to see your child go through a horrible illness. Then, suddenly we became a family with a sick child.
Natasha was diagnosed with Left Ventricular Non-Compaction Cardiomyopathy, a Congenital Heart Defect that caused the left side of her heart to have spongy, porous muscle mass that prevented her heart from pumping efficiently. The condition caused her heart to work extra hard, which also caused Pulmonary Hypertension, a failure to thrive and the enlargement of other strained organs. She was given a 50/50 chance of survival and because there wasn’t a cure, her only real hope of survival was a heart transplant.
As we were in shock and disbelieve, trying to absorb this devastating information, Natasha was whisked onto a stretcher and immediately sent up to the Pediatric Intensive Care Unit, where we stayed with her for an undetermined period of time. We immediately called YANA about our very unexpected extended stay and they arranged accommodations for the rest of us at Jeneece Place next door.
The initial hospital stay ended up being extended for a month. Natasha was closely monitored while being put on some very serious heart management medications, inserted with an NG tube and a nutrition plan was being organized by dietitians. We were taught how to feed, medicate and care for her in this new regime.
We were sent home with a scale, medications, medical supplies and concentrated baby formula and a binder full of medical information and instructions for her new care.
We were then put onto a schedule to return to Victoria General for regular Echos and tests every two weeks. We did that for the next three months, while caring for her at home around the clock in between visits.
During those first three months, Natasha’s case was also being closely monitored by the Cardiology team at BC Children’s Hospital (BCCH) in Vancouver. Once her Cardiologist on the island had exhausted all possible heart management solutions, he referred her directly to her team at BCCH. At first, we did the same routine there, going to BCCH every two weeks, for ECHOs, ECGs, Xrays, bloodwork and examination by the Cardiology Team. Her medications were often adjusted slightly, but during that time there was no real change in her heart condition. It wasn’t expected to get better, but luckily it didn’t get worse. Her heart had to be managed with medication to keep pumping. Her Pulmonary Hypertension did get worse and while she was slowly gaining weight with the help of her team of dietitians, she wasn’t considered strong enough to go through a transplant surgery.
Months went on and Natasha’s medications became more serious. She was fitted with a PICC line to administer a serious heart medication called Milrinone. The tubing from the PICC was then attached to a small pump that we had to carry with Natasha everywhere. This was considered a last resort for Natasha, there wasn’t a lot that doctors could do for her now.
The following months became more involved and our trips to BCCH were a bit longer each time. Natasha had heart biopsies and went through many, many intrusive tests to try to convince surgeons that she was fit to be listed on the BC Transplant List for a new heart. After several months of these tests, we were sent home for Christmas. I was happy that Natasha was allowed to enjoy her first Christmas at home instead of at the hospital.
January came and we were back to BCCH for routine tests and procedures. By Natasha’s first birthday, she was officially second from the top of the list on the BC Transplant List. The next few months would be stressful and uncertain. We had to keep Natasha as strong and as healthy as possible, while we waited an undetermined period of time for a suitable donor heart to become available. If Natasha became too weak, too low in her weight or sick in any way, she would be immediately removed from the Transplant List and we would have to go through the listing process again. This was her last hope of survival. While she wasn’t getting better and she wasn’t getting worse, her days were numbered and we knew that she was constantly in danger of a fatal stroke or cardiac arrest at any time.
Months past and we carried on with our home routine, and regular trips to Vancouver, often staying at the lovely YANA apartments and always so kindly supported by YANA every step. By this time, now that she was listed, Natasha was assigned three home nurses who came into our home and did her medication and care a few days a week to give us a break.
May long weekend came along and not too much had changed with Natasha and now that we had home nurses we didn’t have to go to BC Children’s hospital as much. Only once a month now unless something changed. Natasha had become irritable by this time and began to pass out when she got really upset. The first day, it would happen at nap time and bedtime, but I began to notice it happening in the day that weekend. I also noticed a slight twitching while she was sleeping and we were concerned they were seizures. We called her team at BCCH and they had her and I air lifted there, that night. YANA made arrangements for me to stay at Ronald McDonald House, for when I needed a meal, a shower and a break. Otherwise I had to stay in the ward with Natasha. The following day, my husband and son arrived by car and we were all able to stay there for what was to be an undetermined time again. YANA was again there to support us through this new uncertainty.
We spent the next week at BCCH consulting with neurology who conducted EEGs and sleep tests. She was deemed safe to return home as their reports were inconclusive at the time, but seizures were not expected. We were to keep a close eye on her and head back to BCCH if her symptoms got worse.
On the way home, we bought Natasha a tricycle. The weather was starting to get warmer and since the poor girl had spent the better part of the year inside, either at home or in hospital trying to avoid germs, she deserved some fun outside and at the playground. We assembled the tricycle and Natasha, now 15-months, was so excited to try it out. She first took it for a spin around the house, then, with her big brother steering, we headed out to the playground with it. Natasha had a great day that day, the sun was shining and she just loved her new set of wheels. She enjoyed the swing, took her socks and shoes off and soaked it all in happily.
Three days later: we got: “The Call.” A suitable donor heart became available and we all headed to BCCH for Natasha’s Life Saving Heart Transplant.
It was such a surreal time, just an incredible wave of emotions and yet disbelief. This was the day that we had waited many months for and it had finally arrived. It was both exciting and terrifying at the same time. As soon as we got “The Call,” we called YANA and they made accommodation arrangements for us. We had missed a ferry and ended up on the last ferry of the night, so by the time we got to the hospital, it was midnight. Natasha’s first surgery was at 6am.
She was to have a heart biopsy first, to assess the current condition of her heart and lungs and the following morning have her transplant surgery.
We weren’t impressed by how that trip went, we felt like we should have made it there faster, but the team assured us that we had plenty of time to get there before the donor heart was ready for transplant and so driving and taking the ferry was perfectly fine. We had 12 hours to get there.
Since we had quite a wait for the last ferry, Benjamin decided that it wasn’t a bad thing, he had been looking forward to playing at the terminal playground. There was an amazing sunset that evening and we had so much fun playing with Natasha and Ben at the playground. Little did we know, it would be our last time.
The ferry was quiet that night, not very many cars. The BC Ferries staff, who had come to know us from our many trip across, challenged us to park diagonally on the lower deck this time, just because we could. We were only one of a few cars aboard then. We did and we watched the sun set over the islands and then went to the upper decks for something to eat.
6am arrived quickly and Natasha was swatting the nurses as they tried to turn her to wheel her into the operating room. She just wanted to sleep the poor thing.
Curtains were pulled throughout the ICU and the brave donor was wheeled into the operating room next. I felt a huge amount of respect, love, gratitude and extreme sadness for the donor family. A family who had bravely said yes to donate their child’s organs, to save the lives of multiple children including our daughter Natasha, following their darkest hour of losing their own child.
The waiting during her four-hour surgery was stressful. We paced around the hospital with a block of wood attached to a beeper and were told to go to the waiting room when the beeper went off. Four very long hours with no word on whether our baby girl was okay and whether the new heart was functioning well. Four hours of agony.
Finally, the beeper went off and I am pretty sure that we ran down the long hallways to the waiting room. The surgeon was very calm, soft-spoken and content. The surgery went very smoothly and was a success. He prepared us for what we were about to see and what were about to face in the coming weeks as she recovered. A major surgery like a heart transplant comes with some unpleasant follow-up procedures and graphic sights. Our daughter was heavily sedated and heavily medicated for weeks. She had multiple chest tubes and a breathing tube and, at first, her chest was left open. We had to be strong to be there for her during this terrifying and fragile time.
She was doing very well and we were looking forward to her recovery when she could finally grow and thrive and run without pumps and tubes to worry about. She would be on medication of course for the rest of her life and have regular hospital visits and biopsies, but she would be stronger and able to lead a more normal life overall.
Twelve hours post transplant, the donor heart began to struggle and the surgeon decided that Natasha needed to be put back on to the ECMO machine. The ECMO is a heart and lung machine, it takes over the function of the patient’s natural heart and lungs while in surgery, or in this case, while her heart and lungs settled and regained some strength after a major surgery. During the heart transplant, Natasha also suffered from kidney failure and was on dialysis, which is also very common during a transplant surgery. While her kidneys were expected to fully recover, it caused another danger to her already fragile condition.
Over the next month and half, Natasha had the biggest battle of her life. Through stroke that left her temporarily blind and paralyzed and rejection of the donor organ, fighting fiercely through heart and kidney failure and the continued pulmonary hypertension that was supposed to be relieved following the transplant. It was a month and a half of emotional ups and downs and twists and turns, all the while, Natasha kept pulling through and thriving despite some of her doctors losing confidence. We spent about 12-18 hours a day in the ICU with her. We went in shifts, occasionally taking an afternoon off to have some fun with Ben and visiting family, while she slept.
After 10 days, too many seizures and a stroke, doctors decided that it was too risky to keep Natasha on the ECMO machine any longer. Many of them began to cry and apologize to us, not expecting her to survive being removed from the ECMO. I didn’t believe that this was the end and I let them know my feelings regarding them giving up on her so easily. After being removed from the ECMO, Natasha was in a slightly weaker condition, but soon began to thrive. Her kidneys had recovered fully as well as some of her motor skills and we believe her sight was beginning to come back strongly. She required a lot of therapy from the occupational and physio therapists and the respiratory therapists had to assist her quite a bit with breathing, but she was coming back. We began to consult with rehabilitation therapists and plan for her continued recovery in the ward and eventually at outside facilities.
Every few days, something would come up, whether rejection or kidney issues, but then Natasha would settle and get stronger and stronger. The doctors were finally confident that Natasha was ready to move up to the ward in the coming days. My husband and son went home for a week to check in with work and organize some things at home with the plan to return by the weekend when Natasha would be going to the ward. The week went great, Natasha was breathing better than ever, her vitals were the best ever overall, she was in the best condition ever.
I stayed with her at night until 1 am and then the nurses would encourage me to go for some sleep, because there is very little room for parents in the ICU.
One day, we had visitors in the ICU. First, Shannon and her son Andrew Westerlund. Andrew had received a heart transplant as a baby and was now a teenager in remission from cancer. His mother had contacted me to lend her support during Natasha’s surgery. That afternoon, another special visitor, Elaine Yong, Aaron and Madison McArthur. Madison was born with the same heart defect as Natasha, LVNC and her Transplant and ECMO experience was almost exactly the same as Natasha’s. Aaron is a news anchor for Global and Elaine formerly a reporter, now worked for a private healthcare company. A few months before, Natasha and I were interviewed live by Aaron as part of the 48in48 campaign for organ donation registries. After that, we became friends with them and Madison made many beautiful cards for Natasha over the year. Elaine was a huge support to me especially during the month and a half following Natasha’s heart transplant. Their experience was so similar, and Madison, now 4, had become an amazing example of what transplants can do. This family worked tirelessly for years as very well known and respected advocates and fundraisers for the BC Children’s Hospital and Organ Donation BC. I was happy that Natasha finally got to meet them and that they got to meet her in person.
That night, we Skyped with Les and Ben. It was a bit choppy, due to the lack of cellular signals in the ICU, but at least she could hear their voices. Again, I stayed with her until about 1 am, until she finally settled to sleep. Natasha often struggled to sleep there. With the medication and the constant activity around her, at one point she was awake for several days.
One morning, I headed to the ICU as usual, and passed Natasha’s surgeon in the hall. He was smiling and said she looked good. He had just come off of morning rounds. At her bedside, Natasha was surrounded. The physiotherapist was working with her as she did every morning, and the ICU doctor was fiddling with her IV, apparently her ART line had fallen out during the night. She was also getting urine samples for labs because there was a change in her kidneys overnight. Not being able to get to her right away, I reached over and held her hand and said “Good morning Natasha sweetheart.” Then I chatted with one of the cleaners that we had come to know over our year there.
The physiotherapist had put Natasha in a special chair, which gave her a different perspective and helped strengthen her muscles. I held her hand while they continued to work. All of the sudden Natasha’s face turned pale her oxygen and cardiac levels dropped and she went into cardiac arrest. Nurses rushed to her, several doctors came running down the hall to her bedside. Within seconds, she was surrounded by her Cardiology Team and they all began to take turns administering CPR. There were so many people around her, I decided to leave the ICU to stay out of their way. The social worker came out and got me and brought me back in. I stood at the bottom of her bed, while the medical team continued to work on her. They used an AED and continued CPR. After 45 minutes of trying to save her, our beautiful, happy, silly Natasha had passed away.